
The scope and conceptual framework of our research are illustrated by the figure below, which highlights the dependence between health and socioeconomic factors operating through interactions with the healthcare system.
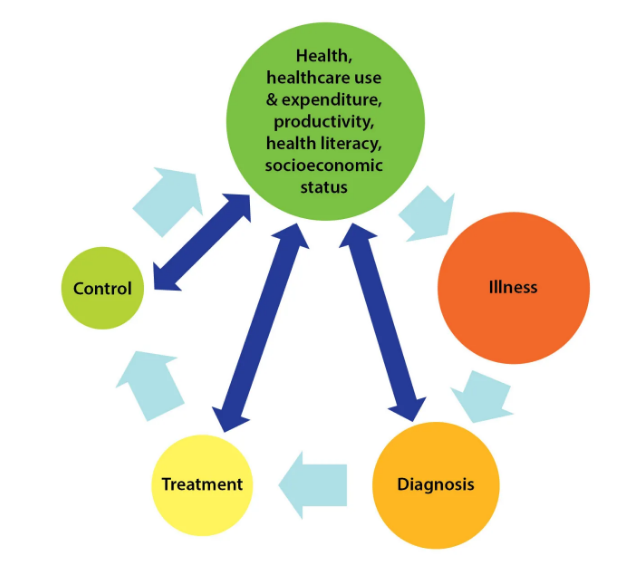
Preventive measures that reduce exposure to these behavioral risk factors are likely to be among the most cost-effective interventions to reduce the ill-health and economic burden arising from non-communicable diseases (NCDs). Without underestimating the importance of socioeconomic determinants of health and public health programs targeting them, this research will purposefully concentrate further downstream on identification of the economic consequences of chronic health problems that have materialized and evaluation of health interventions intended to stop or slow the deterioration in health as a result of such conditions. This focus makes the research relevant to the primary responsibilities of health systems in relation to NCDs – diagnosis, treatment and control.
Inefficiencies that manifest in progressively fewer chronic illnesses being diagnosed, treated and controlled (see the shrinking circles) result in losses of both health and economic output. The circularity of the relationship can give rise to health-related poverty traps with poor health causing poverty and vice versa. The bidirectional arrows between socioeconomic factors and diagnosis, treatment and control of chronic illness represent potential socioeconomic barriers to accessing the healthcare system as well as the out-of-pocket (OOP) cost of using healthcare, which may further exacerbate this poverty trap.
Experiment to identify the impact of improved access to healthcare (diagnosis and treatment) on health and economic outcomes will be structured around the conceptual model of the next figure.
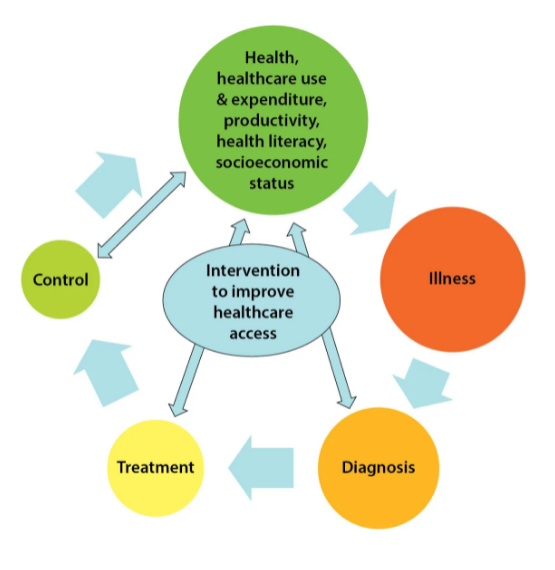
Accessibility and use of healthcare will be exogenously varied to assess the potential of improved healthcare delivery for increased social protection and work productivity, and thus health-led socioeconomic development. We have designed interventions that encourage access to diagnosis and treatment for specific health conditions, weakening the bidirectional causal link between healthcare use and socioeconomic factors (see smaller arrows in the figure). The aim is to diagnose more of the pool of chronic illness and subsequently bring more illness under treatment and control. The size of the circles in the figure just above should increase and shrink less in moving from one stage of the process to the next.
In principle, there is a wide range of potential policy instruments that may potentially achieve this. The exact intervention used to improve healthcare access will depend on the healthcare context of each study site and described in more detail in the country-specific research tabs above.
However, all interventions will in one form or another experimentally manipulate the accessibility of healthcare services by facilitating contact with clinical care providers, and investigate the potential impact of increase accessibility of health services on the dynamic interplay between health events, healthcare use and subsequent health and socioeconomic outcomes and the overall cost-effectiveness of increasing the accessibility of health services from a society’s point of view.
Leave a Reply