
It is important to obtain a full psychiatric and medical history to identify potential causes or contributing factors that may need to be addressed first. Screening for depression is particularly important, given its bidirectional relationship with HSDD. Studies have shown that the risk of sexual dysfunction is increased by 50%–70% among women with depression. Inversely, women with sexual dysfunction have a 130%–210% increased risk for depression (7, 8).
Sexual and/or physical trauma or psychological factors can cause sexual dysfunction and likely require the addition of psychotherapy to the treatment plan. Substance abuse or dependence can also cause sexual dysfunction and should be addressed separately and before interventions specific for HSDD.
Certain antidepressants, such as selective serotonin reuptake inhibitors (SSRIs), serotonin-norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), and monoamine oxidase inhibitors (MAOIs), can cause sexual dysfunction and can be managed with a dose reduction, switch to a different antidepressant, or addition of an antidote. Some antipsychotics, particularly risperidone or first-generation antipsychotics, also cause sexual dysfunction; therefore, it might be useful to obtain a prolactin level in these cases. Treatment recommendations for depression and antidepressant-induced sexual dysfunction are discussed in the following sections.
Providers should also screen for other sexual problems such as arousal or orgasm dysfunction and sexual pain. If present, these conditions might be contributing to or causing the low sexual desire.
It is worth pointing out that numerous medical conditions can cause or contribute to low sexual desire. Hypertension, diabetes, metabolic syndrome, hypothyroidism, urinary incontinence, neurological disorders, and malignancy have all been associated with low sexual desire (6–11).
Several classes of medications have also been associated with low sexual desire (Table 1). Broadly speaking, antihypertensive medications, hormonal preparations, narcotics, psychotropics, and chemotherapeutic agents have all been associated with decreased sexual desire (12). Because of widespread use, it is important to inquire whether the patient is on an oral contraceptive pill (OCP). Checking sex hormone binding globulin (SHBG) and testosterone levels (total and free) might be helpful for this subset of patients, given that OCPs can raise levels of SHBG, which increase binding of testosterone, resulting in a decrease in free and bioavailable testosterone. Although low testosterone is not diagnostic of HSDD, treatment with testosterone may increase sexual desire.

Pathophysiology of HSDD
HSDD is thought to be in part because of an imbalance between excitatory and inhibitory pathways involved in sexual response and behavior in the brain. Generally speaking, dopamine, norepinephrine, testosterone, estrogen, and progesterone are excitatory, whereas serotonin, prolactin, and opioids are inhibitory of sexual desire and response. Pharmacological treatments for HSDD target some of the neurotransmitters and hormones involved in these pathways.
Other factors may also play a role, including psychosocial variables (satisfaction with the relationship, self-image, past sexual experiences among others), aging, menopause, comorbid medical conditions, as well as substances and medications (13, 14).
Treatment
General Considerations
We recommend first assessing the patient’s motivation for treatment and their personal preferences. A variety of treatment options are available for HSDD, including lifestyle modifications and education, psychotherapy, sex therapy, and pharmacotherapy. Treatment should be patient centered. Involving the patient’s partner should be considered. It is also important to assess whether the level of distress is significant enough to consider treatment options that carry the risk of adverse effects.
It is important to screen for contributing psychological factors. Examples include relationship strain, underlying beliefs about sex, history of trauma, and body image issues. In these cases, the appropriate psychotherapy modality to treat these issues should be part of the treatment plan.
If there is concern for an underlying medical condition or medications causing the symptoms, a referral to internal medicine or the patient’s primary care provider should be made. If pain with sexual activity is present, the patient should be referred to gynecology for a targeted examination.
Treatment of HSDD in the Setting of Depression
If depression is present, it should be treated first because untreated major depressive illness is associated with sexual dysfunction. As mentioned earlier, SSRIs, SNRIs, and TCAs can cause sexual dysfunction. For all four classes of antidepressants, sexual dysfunction is numerically but not statistically significantly worse at higher doses (15). Antidepressants that do not cause sexual dysfunction, or that cause it to a lesser degree, are preferred (Table 2). These antidepressants include bupropion and mirtazapine as well as two drugs with serotonin reuptake inhibitor effects as part of their mechanism of action: vortioxetine and vilazodone (16). Vortioxetine recently had a change to its label that states it causes significantly less sexual dysfunction than SSRIs at rates similar to placebo at doses≤10 mg for women and at doses≤15 mg for men. Should sexual dysfunction occur at higher doses, decreasing the dose may improve sexual function.
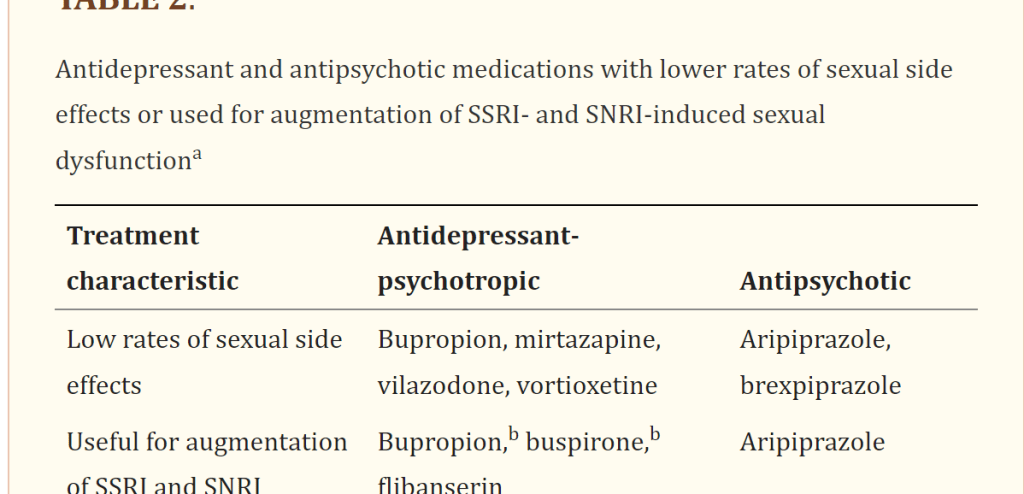
If augmentation with an antipsychotic is needed, aripiprazole and brexpiprazole are preferred options because they have been shown to have a low rate of sexual side effects compared with other antipsychotics (17, 18). If the patient is already on one of these agents, assess whether it is contributing to the sexual dysfunction. Reducing the dose or switching to one of the antidepressants mentioned earlier can be helpful (14, 19). Adjunctive treatment with bupropion (20–22) or buspirone (23, 24) has also been shown to decrease sexual side effects. There is also evidence that adjunctive treatment with mirtazapine can decrease sexual side effects from SSRIs (25).
If insomnia is present, it is recommended that the sleep disturbance be treated independently and to monitor for improvement of sexual symptoms. A study showed that higher insomnia scores and shorter sleep duration were associated with decreased sexual function (26). Flibanserin, which is discussed later, can also potentially help with sleep because of its sedating effects.
Psychotherapy
There are three types of psychological interventions that have been found effective in treating or helping with female sexual dysfunction and symptoms of HSDD.
Behavior therapy attempts to target sexual dysfunction through a combination of communication skills training, education, and sensate focus exercises (27).
Cognitive-behavioral therapy (CBT) can be helpful by challenging unrealistic beliefs contributing to low sexual desire and by changing maladaptive behaviors that perpetuate HSDD. A review of psychological treatments for HSDD found three studies in which CBT was effective for women with HSDD compared with a waitlist control group (28).
Mindfulness-based CBT can help the patient increase awareness of the present moment, minimizing cognitive distractions during sexual activity and enhance awareness of pleasurable sensations (29, 30). Two studies found positive results with mindfulness training among women with HSDD (28). Group mindfulness-based therapy has also been shown to improve sexual desire among women (31, 32).
Resources might be limited depending on the community; therefore, it might be beneficial to cultivate relationships with providers who have expertise in these types of psychotherapy.
Pharmacological Options
Flibanserin. Flibanserin (Addyi) was approved in 2015 by the U.S. Food and Drug Administration (FDA) for treatment of generalized acquired HSDD among premenopausal women.
Its mechanism of action is exerted through serotonin 1A (5HT1A) receptor agonism and serotonin 2A (5HT2A) receptor antagonism. This process reduces serotonin inhibition of excitatory neurotransmitters and thus indirectly increases release of dopamine and norepinephrine (33, 34).
Three randomized, double-blind, placebo-controlled trials demonstrated that flibanserin was efficacious for HSDD symptoms compared with placebo (35–37). All three studies were conducted among premenopausal women, and all were 24 weeks long. Efficacy was measured with the Female Sexual Function Index desire subscale (FSFI-D); Female Sexual Distress Scale–Revised Item 13 (FSDS-R13), which measures distress associated with sexual desire; and Satisfying Sexual Events (SSE), as determined by the woman. All efficacy endpoints in the phase 3 studies demonstrated statistical significance in change from baseline to endpoint over placebo. Relative to placebo, flibanserin had an effect size of 0.29–0.44 (desire) and 0.24–0.44 (distress). Improvement was seen after 4 weeks of daily dosing. One study found that 50 mg given at bedtime was efficacious (36); however, another study did not find this dose to separate from placebo (35). All studies found that 100-mg daily dosing was effective in approximately 50% of women. Responders found the effect to be clinically meaningful.
A 52-week open-label extension study found that flibanserin was safe and well tolerated. Sexual function improved among participants who were initially nonremitters and was maintained over time in remitters (38).
Even though flibanserin is not indicated for postmenopausal women, evidence suggests that it is also effective among this population (39). The recommended dose is 100 mg given once daily at bedtime. When assessing for improvement, one should inquire about changes in sexual desire, reduction in distress related to sexual dysfunction, and satisfaction with the treatment. If no improvement occurs after 8 weeks, one should consider discontinuing this medication.
Flibanserin is safe to use concomitantly with SSRIs and SNRIs. A small randomized, placebo-controlled trial demonstrated no serious adverse effects and no instances of suicidal ideation and behavior when combining flibanserin 100 mg daily with a stable SSRI or SNRI treatment regimen (40).
The most common adverse reactions (incidence≥2%) include dizziness, somnolence, nausea, fatigue, insomnia, and dry mouth. Hypotension and syncope have been reported, and its package insert has a warning for these conditions (41).
Previously, concomitant use with alcohol was contraindicated and required a risk evaluation and mitigation strategy (REMS) because of concerns for orthostatic hypotension and syncope. Studies have demonstrated that it is safe to use flibanserin with alcohol. Taking this medication 2, 4, and 6 hours after ethanol consumption did not increase the incidence of hypotension, orthostatic hypotension, or syncope compared with flibanserin or ethanol alone (42–44). Thus, the REMS program was discontinued, and the label was changed to recommend not using flibanserin within 2 hours of alcohol consumption.
Flibanserin does not appear to prolong the corrected QT interval (41). It is primarily metabolized by cytochrome P450 3A4 (CYP3A4) and cytochrome P450 2C19 (CYP2C19); therefore, one should review the patient’s medication list for moderate and strong inhibitors or inducers of these enzymes. The risk of severe hypotension is increased with CYP3A4 inhibitors. Examples of strong CYP3A4 inhibitors include clarithromycin, HIV protease inhibitors, ketoconazole, and grapefruit juice. Strong inducers of CYP3A4 include phenytoin, phenobarbital, rifampin, carbamazepine, and St. John’s wort. Strong inhibitors of CYP2C19 include fluoxetine, fluvoxamine, proton-pump inhibitors, antifungals, and benzodiazepines.
Flibanserin can increase the concentration of drugs transported by P-glycoprotein (P-gp). It is recommended to increase monitoring of concentrations of drugs transported by P-gp that have a narrow therapeutic index, such as digitalis and rapamycin.
The use of flibanserin is contraindicated in hepatic impairment because there is a 4.5-fold increase to flibanserin exposure in this population. Its use in pregnancy and breastfeeding has not been studied; therefore, it is not recommended.
Currently, this medication costs $99 per month without insurance. However, discounts as low as $20 per month for patients with commercial insurance can be found at https://addyi.com/howtosave.
Bremelanotide. Bremelanotide (Vyleesi) was approved in 2019 by the FDA for treatment of generalized acquired HSDD among premenopausal women.
Bremelanotide is a melanocortin 4 receptor (MC4R) agonist. Neurons expressing the MC4R are present throughout the central nervous system (45). The mechanism by which bremelanotide improves HSDD is unknown, but it is thought to increase excitation by enhancing dopamine and norepinephrine activity.
The FSFI-D, item 13 of the Female Sexual Distress Scale-Desire/Arousal/Orgasm (FSDS-DAO), and SSE were also used in the phase 3 studies and demonstrated that bremelanotide is significantly more effective than placebo (46). The combined effect size for the two phase 3 studies relative to placebo was 0.39 for FSFI-D and 0.27 for FSDS-DAO item 13. The response rate for bremelanotide was 58.2% versus 35.6% for placebo in the integrated phase 3 data set. This response was considered clinically meaningful by the study participants. An extension study also showed that after 52 weeks, response to this medication was maintained (47).
The recommended dose is 1.75 mg administered subcutaneously in the abdomen or thigh via an autoinjector, on an as-needed basis. Patients should inject the medication at least 45 minutes before a sexual encounter. It is not recommended to use more than one dose within 24 hours, or more than eight doses within 1 month.
As with flibanserin, one should inquire about changes in sexual desire, reduction in distress related to sexual dysfunction, and satisfaction with the treatment to assess for treatment response. If no improvement occurs after 8 weeks, one should consider discontinuing this medication.
The most common adverse reactions (incidence≥4%) include nausea, flushing, headache, vomiting, and adverse site reactions. Nausea is the most common adverse reaction. In placebo-controlled trials, 40% of patients receiving bremelanotide reported nausea compared with 1% of patients receiving placebo. Hyperpigmentation of the face, gingiva, and breasts has also been reported (48).
Bremelanotide can cause transient increases in blood pressure, and it is contraindicated in uncontrolled hypertension. Providers should consider the patient’s cardiovascular risk and ensure that blood pressure is well controlled.
Of note, bremelanotide can significantly decrease the absorption of oral naltrexone, and its concomitant use is not recommended. The use of intramuscular naltrexone can be an alternative for this subset of patients.
This medication also has cost savings available online at https://www.vyleesi.com/getting-started. With these discounts, the current cost varies between $0 and $99 per 4-pack of autoinjectors.
Testosterone. Although approved in Europe for treatment of HSDD among women with surgical menopause, it is an off-label treatment option in the United States. Studies on testosterone for HSDD have been largely conducted among women who have undergone natural or surgical menopause. Evidence is lacking for premenopausal women, and should a woman become pregnant, fetal exposure may be associated with significant negative consequences.
Three randomized, double-blind, placebo-controlled trials have shown that a 300-μg/d transdermal testosterone patch was superior to placebo in improving symptoms of HSDD. Women who received this medication reported improvement in satisfying sexual events as well as a decrease in levels of distress. Lower testosterone doses were not effective (49–52). This product was not approved in the United States because of lack of information about long-term consequences. These concerns have not been borne out in use in other countries.
Transdermal use is recommended. Oral or intramuscular preparations are not recommended because of high variability of absorption, which typically achieves supraphysiologic levels and increases the risk of adverse effects.
Improvement of symptoms is expected within the first 3 months of treatment. If the patient does not experience improvement in symptoms after 3–6 months, consider discontinuing treatment (53).
The most common side effects are acne, application site reactions, breast pain, headache, and hirsutism. In several studies, liver function, lipid profile, hematologic tests, and clotting measures remained essentially unchanged (49–52).
Baseline and follow-up testosterone levels should be obtained. Levels should be maintained within normal ranges. Short-term safety data are reassuring when testosterone levels are maintained within normal levels (54). However, long-term data are limited to observational studies, including safety data with regard to breast cancer and cardiovascular events (55).
Testosterone formulations for women are not widely available. Most clinicians will have to use topical formulations for men but at a much lower dose, generally one-seventh to one-tenth of approved doses for men to avoid virilization. Compounded formulations are another option.
Leave a Reply