Global healthcare has entered a transformative phase. According to an innovative map and evidence-based data provided by StartUs Insights (2021), many countries and healthcare organizations will increase investment between 2021 and 2030 to acquire and integrate new technologies and health management ideas that add value to global healthcare delivery. Technology-reliant treatments will also experience much wider acceptance from patients. But at the same time, demographic trends such as the increasing number of middle class and aging population create a heavy burden on global health providers. Demand for health care services will expand over time. And threats from new waves of COVID-19 underscore the need improve global health systems. Therefore, every country has a responsibility to establish a robust health innovation ecosystem that leverages both human and material (intangible) resources to adapt with global health challenges and transform clinical services.
Figure 5.1: 2021 Trends in Healthcare Innovation
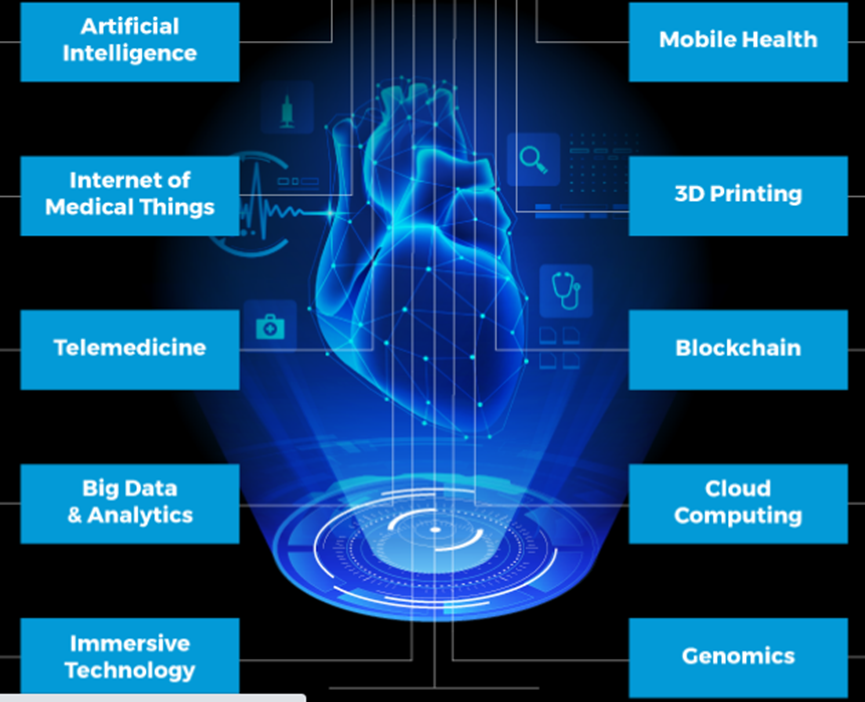
Based on the Healthcare Innovation Map from StartUs Insights (2021), many health organizations are exploring artificial intelligence (AI) and the internet of medical things (IoMT) to provide real-time, non-stop, and remote monitoring devices that improve the quality of patient care. Telemedicine solutions make clinical services accessible when—or in areas where—health providers are not available for direct contact or frequent visits. 3D Printing (specifically bioprinting) is used to develop high-quality prosthetics and tissue and organ transplants while reducing the chances of draft rejection as well as lessening the burden on donors. The Big Data and analytics use coordinated processes to study both structured or unstructured medical data (including biomedical literature) to gain previously unknown insights in medicine and health care management. Similarly, global healthcare systems now explore augmented reality (AR), virtual reality (VR), and mixed reality (MR) to transform user experience in digital therapy. It is also important to add that blockchain and cloud computing—buoyed by unprecedented digitization in global healthcare—have changed the ways clinical data is collected, stored, and used in care management. Interestingly, the growth of nanomedicine, genomics, and regenerative medicine have significantly enhanced and advanced personalized healthcare provided in many health organizations.
Figure 5.2: Percentage of Global Health Innovation Trends in 2021

| Healthcare Innovation | Percentage (%) |
| Artificial Intelligence (AI) | 18% |
| TELEMEDICINE | 12% |
| IMMERSIVE TECH | 11% |
| MOBILE HEALTH | 8% |
| IoMT | 17% |
| BIG DATA & ANALYTICS | 11% |
| 3D PRINTING | 7% |
| BLOCKCHAIN | 6% |
| CLOUD COMPUTING | 5% |
| GENOMICS | 5% |
Increasing levels of income and education are strengthening wide acceptance and adoption of health innovation across developed and developing countries. But there are concerns for disparity in technology adoption and the costs of universal healthcare. For example, governments in the African continent have different health needs as well as unequal budgetary allocations to the health sector, and some policymakers are driven by political objectives rather than innovation and delivery of primary care to every individual and household as promoted in WHO’s Health for All agenda.
Poor innovation management practices in many developing countries like Nigeria, where emphasis is on strict implementation of health policies formulated without input from local researchers, has been a bane to economic growth and development. Various health development programs in the country were neither patient-centred nor aligned with healthcare models (e.g. the Bismarck, Beveridge or NHIS care models) that are proven to be more effective, accessible, and affordable in developed economies. But Nigeria has abundant human and natural resources it could explore to benefit from health innovation. The problem is lack of political will among leaders, and this limits the potential for innovative treatments in public-owned health facilities. Consequentially, a large number of care users (patients) are left vulnerable to the extortive out-of-pocket payment model implemented in private health organizations.

Leave a Reply